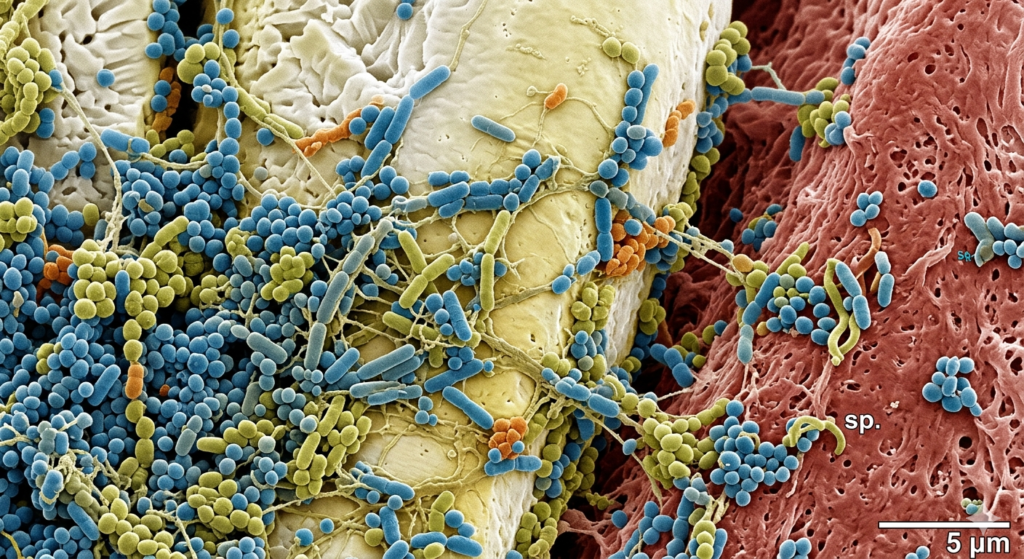
Oral Microbiome: The Surprising Link Between Gum Health and Heart Disease
The 2026 Wake-Up Call: When Health Tracking Becomes Exhausting
In 2026, many people feel worn out by constant health metrics. Smart rings track sleep stages. Watches track heart rate variability. Apps measure glucose and steps. Yet even with all that data, many still feel like something important is missing.
Ironically, one of the biggest signals of long-term health might not come from a wearable at all.
It might come from your gums.
Researchers and clinicians are paying renewed attention to the oral microbiome the ecosystem of bacteria living in your mouth. What used to be framed simply as “brush and floss” hygiene is now part of a broader conversation about metabolic resilience, nervous system medicine, and whole-body inflammation.
And the connection drawing the most attention right now?
The relationship between gum health and heart disease.
Your mouth is not separate from the rest of your body. It’s the entrance to the digestive system, a hub of immune activity, and a place where microbial balance can influence the bloodstream.
Understanding this connection doesn’t require perfection or fear. Instead, it’s about restoring ancestral habits, supporting circadian rhythm, and giving your body the conditions it needs to regulate itself.
Let’s break down what the science and practical experience are showing.
Understanding the Oral Microbiome and Heart Health
The oral microbiome is the community of bacteria living in the mouth. When balanced, it supports healthy gums and immune defense. When disrupted, harmful bacteria may enter the bloodstream through inflamed gums, contributing to systemic inflammation that researchers increasingly associate with cardiovascular health risks.
The mouth hosts more than 700 species of microbes.
Most are beneficial. They help:
- Start digestion
- Maintain pH balance
- Protect teeth and gums
- Support immune signaling
Problems arise when the microbial environment shifts toward inflammatory bacteria. This imbalance is often called oral dysbiosis.
Signs of dysbiosis may include:
- Bleeding gums
- Persistent bad breath
- Gum tenderness
- Plaque buildup
- Gum recession
When gums become inflamed, microscopic openings can allow oral bacteria to enter circulation.
This doesn’t mean gum issues automatically cause heart disease. But the overlap between gum inflammation and cardiovascular risk markers has become difficult to ignore.
Why Gum Inflammation Can Affect the Heart
Inflamed gums may allow oral bacteria and inflammatory molecules to enter the bloodstream. These microbes can trigger immune responses linked with arterial inflammation. Over time, chronic inflammation is associated with reduced cardiovascular resilience and changes in blood vessel function.
Several biological pathways explain the connection.
1. Systemic Inflammation
Gum inflammation increases inflammatory signaling molecules.
These signals don’t stay local. They circulate through the bloodstream and may influence:
- Blood vessel lining
- Immune responses
- Plaque formation in arteries
2. Bacterial Migration
Certain oral bacteria have been identified in arterial plaque samples.
This suggests bacteria from the mouth may travel through the bloodstream and influence cardiovascular tissue.
3. Immune System Stress
The immune system reacts continuously to oral inflammation.
Over time, this ongoing response may contribute to chronic inflammatory load, which affects metabolic resilience.
The 2026 Health Perspective: From Over-Optimization to Regulation
Modern wellness thinking is shifting from constant health optimization toward supporting the body’s natural regulatory systems. Instead of chasing perfect metrics, the focus now emphasizes nervous system balance, metabolic flexibility, and daily rhythms that support microbial harmony in the mouth and body.
For years, the health world emphasized optimization:
- Perfect macros
- Constant supplements
- endless biohacking metrics
Now, a quieter trend is gaining traction.
Regulation over optimization.
Many clinicians now emphasize:
- Nervous system regulation
- Circadian rhythm alignment
- Whole-food synergy
- ancestral habits
Why?
Because the microbiome oral and gut responds strongly to daily rhythm and stress signals.
Chronic stress alters:
- saliva composition
- immune signaling
- microbial balance
A regulated nervous system supports:
- healthier saliva flow
- better immune tolerance
- improved microbial diversity
Which means gum health often improves when the whole system stabilizes.
Five Key Factors That Shape the Oral Microbiome
How circadian rhythm affects oral bacteria balance
Circadian rhythm influences saliva production, immune signaling, and microbial activity in the mouth. When sleep cycles are consistent, saliva helps regulate oral bacteria. Disrupted sleep or late-night eating may reduce this protective effect and increase the risk of gum irritation.
Saliva is one of the mouth’s most underrated defenses.
It helps:
- neutralize acids
- wash away bacteria
- deliver antimicrobial compounds
But saliva production follows a circadian rhythm.
Healthy rhythm patterns include:
- Higher saliva flow during the day
- Lower flow during sleep
- Strong immune signaling overnight
Disruptions happen when people:
- snack late at night
- stay awake past natural sleep cycles
- consume sugary drinks before bed
Over time, these habits shift the oral ecosystem.
Supporting circadian rhythm supports oral microbial balance.
The role of metabolic resilience in gum health
Metabolic resilience refers to the body’s ability to process nutrients and maintain stable energy. When metabolic health is stable, inflammation tends to remain lower. Stable blood sugar levels may help reduce gum irritation and support a balanced oral microbiome.
Blood sugar swings affect more than energy.
They influence:
- inflammatory signaling
- microbial growth
- immune activity in gum tissue
High sugar exposure feeds certain oral bacteria that produce acids and irritate gums.
Metabolic resilience grows through:
- balanced meals
- fiber-rich foods
- movement after eating
- consistent sleep timing
This metabolic stability helps protect both gum tissue and cardiovascular health markers.
Whole-food synergy and the oral microbiome
Whole-food synergy describes how nutrients in natural foods work together to support biological systems. Vitamins, minerals, and phytonutrients in whole foods can support gum tissue, immune signaling, and microbial diversity in the mouth.
Rather than focusing on single nutrients, modern nutrition research highlights food synergy.
Foods that support oral health include:
- leafy greens
- fermented foods
- crunchy vegetables
- fatty fish
- nuts and seeds
These foods contribute nutrients like:
- vitamin C
- omega-3 fats
- polyphenols
- minerals needed for tissue repair
Whole foods also encourage chewing, which stimulates saliva production.
That mechanical action alone supports oral balance.
Nervous system medicine and gum inflammation
Nervous system medicine focuses on how stress regulation affects physical health. Chronic stress can alter saliva, immune activity, and inflammatory signaling in gum tissue. Practices that calm the nervous system may indirectly support healthier oral microbial balance.
Stress changes body chemistry quickly.
During prolonged stress:
- cortisol rises
- immune responses shift
- saliva composition changes
This can make gums more reactive.
Helpful practices often include:
- morning sunlight exposure
- slow nasal breathing
- gentle movement
- regular sleep timing
These habits support parasympathetic nervous system activity, which promotes repair and immune balance.
Ancestral habits that supported oral health
Many ancestral cultures maintained strong oral health without modern dental products. Daily habits such as fibrous diets, sunlight exposure, and consistent sleep cycles supported microbial balance and gum integrity through natural chewing, saliva flow, and immune regulation.
Traditional lifestyles often included:
- fibrous plant foods
- fermented foods
- outdoor daylight exposure
- minimal processed sugar
These habits supported oral ecology naturally.
Chewing tough foods like raw vegetables and roots stimulated saliva and cleaned teeth mechanically.
While modern dentistry is valuable, reviving supportive daily habits adds another layer of protection.
Table 1: Nutrient Density & Bio-Availability Comparison
| Food | Key Nutrients | Oral Health Benefit | Bio-Availability Notes |
|---|---|---|---|
| Spinach | Vitamin C, folate, magnesium | Supports gum tissue repair | Fat improves absorption |
| Sardines | Omega-3s, calcium, vitamin D | Supports anti-inflammatory pathways | Highly absorbable minerals |
| Carrots | Fiber, beta-carotene | Stimulates saliva and mechanical cleaning | Raw chewing increases benefit |
| Yogurt (fermented) | Probiotics, calcium | Supports microbial diversity | Live cultures most beneficial |
| Pumpkin seeds | Zinc, magnesium | Supports immune signaling | Best absorbed when soaked or roasted |
The Modern Rhythm Protocol
The Modern Rhythm Protocol focuses on daily patterns that support circadian rhythm, metabolic resilience, and oral microbial balance. It combines morning light exposure, balanced meals, hydration, and calming evening routines to promote gum health and cardiovascular resilience through consistent daily rhythm.
This routine isn’t about perfection.
It’s about rhythm.
Morning Routine
1. Morning light exposure ☀️
Within 30 minutes of waking:
- spend 5–10 minutes outside
- allow natural light to reach your eyes
This anchors circadian rhythm and supports hormonal balance.
2. Hydration
A glass of water supports saliva production after sleep.
3. Gentle oral care
- brushing
- flossing
- tongue cleaning
This resets the oral environment after overnight bacterial growth.
4. Balanced breakfast
Focus on protein, fiber, and healthy fats to support metabolic resilience.
Example:
- eggs
- sautéed greens
- whole grain toast
- yogurt
Midday Rhythm
1. Chew real foods
Crunchy vegetables and whole foods stimulate saliva.
2. Move after meals
A short walk supports blood sugar balance and metabolic flexibility.
Evening Routine 🌙
1. Early dinner timing
Eating earlier allows digestion and microbial rhythms to settle before sleep.
2. Calm the nervous system
Examples:
- slow breathing
- stretching
- journaling
- screen-free time
3. Night oral care
Brushing and flossing remove food particles that bacteria feed on overnight.
Table 2: 7-Day Bio-Harmony Routine Tracker
| Day | Morning Light | Whole-Food Meals | Calm Practice | Evening Oral Care |
|---|---|---|---|---|
| Monday | ✓ | ✓ | ✓ | ✓ |
| Tuesday | ✓ | ✓ | ✓ | ✓ |
| Wednesday | ✓ | ✓ | ✓ | ✓ |
| Thursday | ✓ | ✓ | ✓ | ✓ |
| Friday | ✓ | ✓ | ✓ | ✓ |
| Saturday | ✓ | ✓ | ✓ | ✓ |
| Sunday | ✓ | ✓ | ✓ | ✓ |
Tracking rhythms not perfection helps reinforce supportive habits.
The Verdict
Healthy gums are more than a dental concern. They reflect the balance of the oral microbiome, immune activity, and daily lifestyle rhythms. Supporting circadian rhythm, metabolic resilience, and whole-food nutrition can help maintain oral balance that benefits both gum health and long-term cardiovascular wellness.
The mouth is a gateway ecosystem.
When gums are inflamed, it often signals deeper imbalance involving:
- stress
- diet
- sleep rhythm
- microbial diversity
Instead of chasing endless optimization metrics, the more helpful approach for many people in 2026 is simple:
support the rhythms your body already understands.
That includes:
- consistent sleep cycles
- nourishing whole foods
- calming the nervous system
- daily oral care
Small habits practiced consistently often outperform complicated health routines.
And sometimes, the simplest signal of whole-body wellness is a smile with healthy, calm gums.
Quick FAQ
Does gum disease increase heart disease risk?
Research shows an association between gum inflammation and cardiovascular risk markers. Inflamed gums may allow bacteria and inflammatory molecules to circulate through the bloodstream. Maintaining healthy gums may support overall cardiovascular wellness as part of a balanced lifestyle approach.
How does the oral microbiome affect the body?
The oral microbiome influences digestion, immune signaling, and inflammation. When balanced, beneficial bacteria help protect teeth and gums. When disrupted, harmful microbes may increase inflammation and affect other systems, including metabolic health and cardiovascular function.
Can improving gum health support metabolic resilience?
Healthy gums reduce inflammatory stress on the body. Lower inflammation supports metabolic resilience, which helps stabilize energy levels and blood sugar regulation. Lifestyle habits that support oral health like whole foods and good sleep also support metabolic balance.
Are natural foods helpful for oral microbial balance?
Whole foods such as vegetables, fermented foods, and mineral-rich seeds support gum tissue and microbial diversity. Chewing fibrous foods stimulates saliva, which naturally regulates bacteria and protects the oral environment.
What daily habit most supports gum health?
Consistent oral hygiene combined with circadian rhythm alignment is one of the most helpful strategies. Brushing, flossing, balanced meals, adequate sleep, and stress regulation create conditions where beneficial oral bacteria can thrive.










